Glaucoma: Immune Cells Play Key Role in Regulating Eye Pressure
Exciting new research highlights how immune cells help protect vision. Researchers discovered that resident macrophages act as a “cleanup crew” in the eye’s drainage tissue. When these cells were removed in experimental models, fluid accumulated and intraocular pressure increased. The findings suggest a promising new immune target for future therapies aimed at preventing glaucoma.
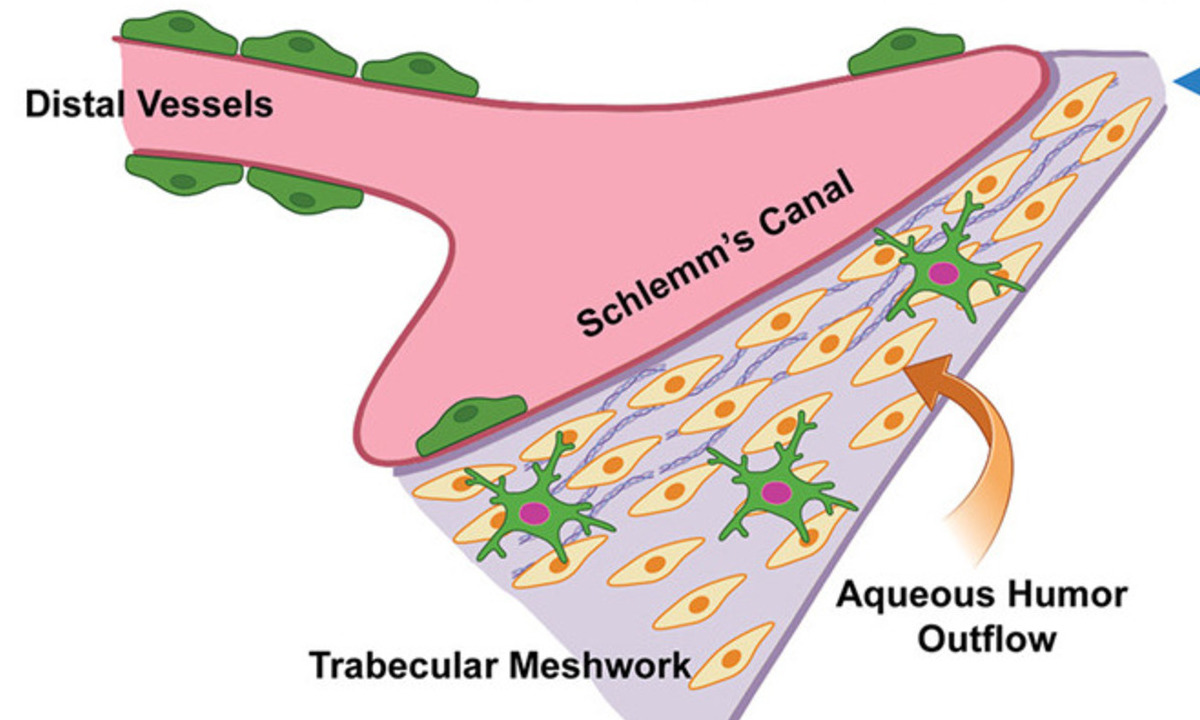
When the eye’s drainage system clogs, pressure builds up and causes damage. The pressure can lead to glaucoma and vision loss.
New research, published in the journal Immunity, reveals that a specialized set of immune cells act as the cleanup crew, pointing to a promising new target for therapies to prevent glaucoma.
These immune cells—known as resident macrophages—reside in the eye’s drainage tissues. Using macrophage lineage tracing and fluorescent cell tracking in mouse models, researchers found that long-lived resident tissue macrophages are particularly enriched in the trabecular meshwork and Schlemm’s canal, where they play a critical role in maintaining IOP homeostasis.
“The only way we can treat glaucoma is by lowering the eye pressure, yet we still have patients who go blind despite current treatments,” said Katy Liu, M.D., Ph.D., lead author of the study and assistant professor in the Department of Ophthalmology at Duke University School of Medicine.
“This research helps us understand the role of the immune system in regulating eye pressure,” Liu said.
In the study, researchers tracked fluorescently tagged resident macrophages in mouse eyes. When they selectively removed these cells, the eye’s drain became clogged, fluid built up, and eye pressure increased.
In the study, researchers tracked fluorescently tagged resident macrophages in mouse eyes. When they selectively removed these cells, the eye’s drain became clogged, fluid built up, and eye pressure increased. The rise in outflow resistance was associated with dysregulated extracellular matrix turnover in the resistance-generating tissues of the trabecular meshwork.
“Our findings show that resident macrophages are essential for maintaining healthy eye pressure,” said Liu. “Disruption of this system may contribute directly to the development of glaucoma.”
This discovery could lead to the development of future glaucoma treatments. The next step is to do research that identifies these resident macrophages in human eye tissue.
“Now we have a specific target for developing new therapies that can normalize the eye pressure and stop vision loss, in contrast to current medications that do not target the source of disease,” said W. Daniel Stamer, Ph.D., corresponding author, Joseph A.C. Wadsworth Distinguished Professor of Ophthalmology, and Co-Vice Chair for Basic Science Research.
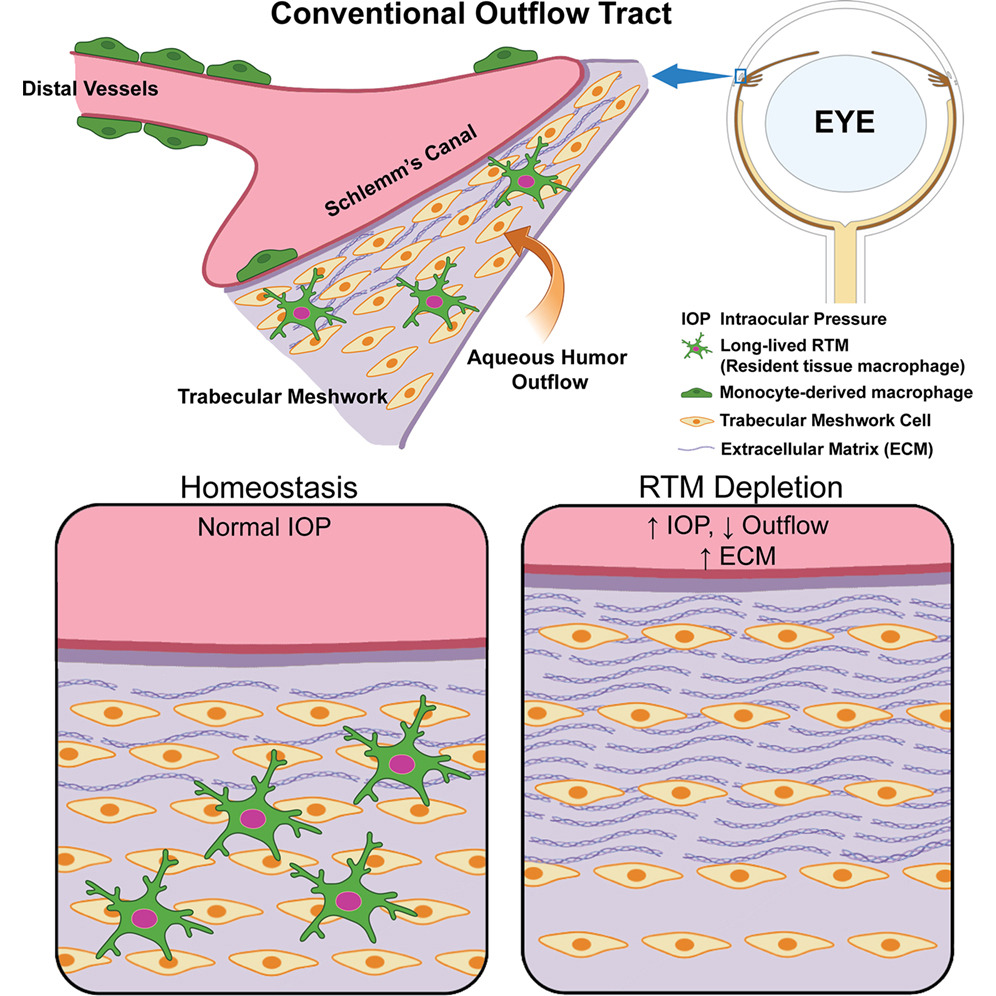
Graphical abstract. Image: Immunity
The Duke Eye Center has a long history of breakthroughs in glaucoma, including research that led to FDA-approval of the first new drug to treat glaucoma in 20 years.
“This discovery is a major step forward in understanding how the immune system contributes to the regulation of eye pressure,” said Daniel Saban, Ph.D., co-corresponding author, Joseph A.C. Wadsworth Distinguished Professor of Ophthalmology, and Vice Chair of Research Strategy in the Department of Ophthalmology. “This research builds on Duke's strong history of turning laboratory findings into real treatments for patients.”
Katy C. Liu et al., Resident tissue macrophages maintain intraocular pressure homeostasis, Immunity, 2026, https://doi.org/10.1016/j.immuni.2026.01.025.
Source: Duke University School of Medicine.